Muscular Sanity: The Language of Pain in Literature
Emily Wells on the language of pain in literature.
By Emily WellsMarch 14, 2018
“ENGLISH,” VIRGINIA WOOLF WRITES in “On Being Ill,”
which can express the thoughts of Hamlet and the tragedy of Lear, has no words for the shiver or the headache […] The merest schoolgirl when she falls in love has Shakespeare or Keats to speak her mind for her, but let a sufferer try to describe a pain in his head to his doctor and language at once runs dry.
Woolf seeks to establish illness as a serious project in literature, which “does its best to maintain that its concern is with the mind; that the body is a sheet of plain glass through which the soul looks straight and clear, and, save for one or two passions such as desire and greed, is null, negligible, and non-existent.”
However, even in this essay on illness, Woolf only hints at the mental and physical ailments that plagued her throughout her life, asserting that, in the matter of disease, “we go alone, and like it better so. Always to have sympathy […] would be intolerable.” Though she potently explores states of illness in her fiction — Rachel’s delirious, raging fever in The Voyage Out, Rhoda’s madness in The Waves, and Septimus’s suicidal mania Mrs. Dalloway — in describing pain explicitly and specifically her own, language does appear to run dry.
Considering this disparity between her fictional and nonfictional treatments of pain, we must ask, is the “running dry” a failure of language, or of the will? Does Woolf’s reticence owe more to the shame that goes hand in hand with sharing one’s pain than to a weakness in the language itself? Perhaps language fails us only when we wish to express our pain, rather than the pain of others. In her 1985 volume The Body in Pain: The Making and Unmaking of the World, Elaine Scarry echoes Woolf’s lamentations at the limits of language:
Whatever pain achieves, it achieves in part through its unsharability, and it ensures this unsharability through its resistance to language […] Physical pain does not simply resist language but actively destroys it, bringing about an immediate reversion to a state anterior to language, to the sounds and cries a human being makes before language is learned.
Scarry also notes that the language used to describe the physical pain experienced by the individuals she has interviewed often comes from others speaking on their behalf. To the person in pain, there is no reality besides that pain. The effect of this reality-defining pain on an individual identity is modeled in Meghan O’Rourke’s most recent poetry collection, Sun in Days, a poignant meditation on chronic illness:
I discovered what I had always naturally called I was really no longer an “I.”
It changed all the time — in fact, entirely receded as a coherent notion — according to something happening in my cells that no one could identify …
Walking, teaching, writing, I experienced myself as categorically fraudulent.
This experience of categorical fraudulence, in which one lacks the exact word for an experience, may force a writer into the realm of metaphor. Yet in Illness as a Metaphor, Susan Sontag takes issue with disease metaphors. “I want to describe not what it’s really like to emigrate to the kingdom of the ill and to live there,” she writes, “but the punitive or sentimental fantasies concocted about that situation; not real geography but stereotypes of national character.” Throughout, Sontag challenges psychological abstractions that do more harm than good:
We are not being invaded. The body is not a battlefield. The ill are neither unavoidable casualties nor the enemy […] About that metaphor, the military one, I would say, if I may paraphrase Lucretius: Give it back to the war-makers.
Sontag’s condemnation of metaphor is refreshing and even salutary, but what language is left for those who suffer from diseases that don’t have a precise scientific designation? Can writers who wish to convey the nuanced experience of being in an ill body resist metaphor? In any event, relying on seemingly precise definitions may actually obscure the true meaning of an experience.
This is particularly evident in the case of female “hysteria,” a 19th-century designation that has since been written off as absurd and misogynistic — the Greek hustéra, or womb, is the root of hysteria, encoding in language the assertion that the female body is more fragile and volatile than its male counterpart. The alleged disease encompassed a wide range of conditions, including emotional excess, sexual desire, seizures, anxiety, and eating disorders. Jean-Martin Charcot, the leader in hysteria research at the Salpêtrière hospital in Paris, hypothesized that it the illness was caused by a lesion — which he never found. But in Medical Muses: Hysteria in Nineteenth-Century Paris, Asti Hustvedt insists that the diagnosis was useful:
The Salpêtrière provided a language — the language of hysteria — that allowed them to articulate their distress […] To what degree their disease was socially determined and to what degree it was physically determined is impossible to say. If they showed up at a hospital today, suffering from the same symptoms, they would probably be diagnosed with schizophrenia or conversion disorder or bipolar disorder […] I am convinced that [the women treated at the Salpêtrière] were neither frauds nor passive receptacles of a sham diagnosis. They really did “have” hysteria. Located on the problematic border between psychosomatic and somatic disorders, hysteria was a confusion of real and imagined illness.
Retrospectively, the widespread phenomenon of hysteria is largely considered a cultural disease, existing only within a specific historical context. However, Hustvedt asserts that the stories of the medical woes of modern women “seem to belie [hysteria’s] current status as a defunct disease,” citing mass psychogenic illness outbreaks — “another name for mass hysteria,” she says — and many contemporary illnesses, such as chronic fatigue syndrome.
Hustvedt is right to insist that the experience of the suffering person is real. While critical of Charcot’s methods throughout the book, she lauds him at the end for having acknowledged hysteria as a true illness: “he did nothing less than articulate a new paradigm for illness, one that superseded the tenacious mind-body model that we are still muddling about in.” Still, calling the hysterics’ condition “a confusion of real and imagined illness” may perpetuate the relegation of symptoms without (known, observed, identifiable) biological markers into the category of the unreal.
It was, after all, the unfound lesion that Charcot believed would mark hysteria as real. Charcot’s insistence upon examining hysteria in a purely biological framework perpetuated a harmful paradigm, asserting that women were somehow biologically prone to hysteria. It was only near the end of his life that he decided that hysteria was a psychological disease. Charcot worked in the late 1800s, an era which marked a turn after which behaviors formerly thought of as religious expression were recast as symptoms of illness. Self-starvation and mutilation of the flesh, even when carried out by a religious patient professing penance, were relegated to the list of hysterical symptoms. In a sense, the medical world sought to “save” the women in a capacity formerly left to the church, a practice largely perpetuated by the assertion that hysteria was a purely biological disease. By 1883, the beds in the Salpêtrière, previously named after saints, were renamed after scientists.
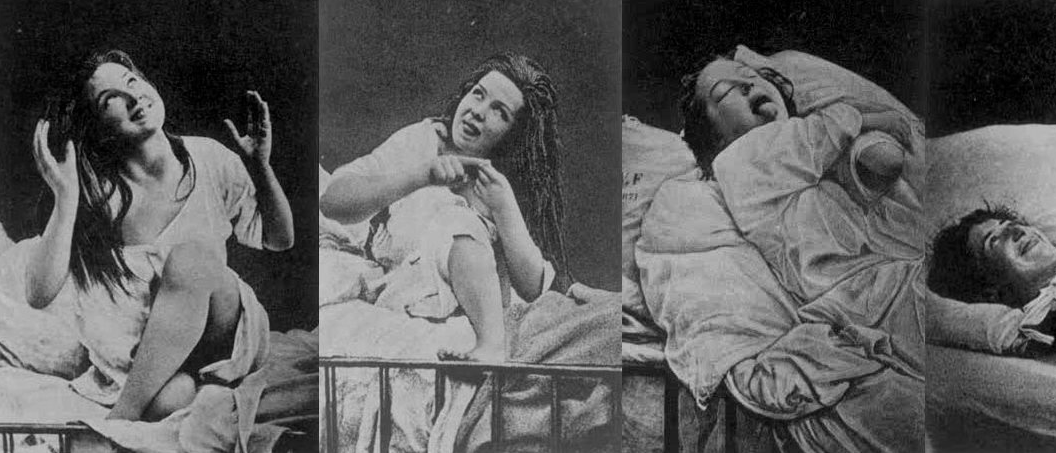
A young woman named Louise Augustine Gleizes was Charcot’s most performative patient, and thus, his most famous. Her illness was eroticized by Charcot, who used hypnosis, bright lights, and prodding to guide her to reenact her spectacular symptoms of spasms, cries, and hallucinations, and hold them long enough to be captured by a camera. Foucault called the Salpêtrière “a machinery for incitement.” But Augustine inflected the photographs with too much life and personality for them to serve as pure medical documents as they were intended — the glamour of the pictures has in some respects overshadowed Charcot’s medical contributions.
Like Augustine, literature’s women-in-pain are frequently performative: Miss Havisham dwells in her wedding dress until it burns, Anna Karenina jumps into the train’s path, Esther in The Bell Jar waits to die under her childhood home. As I work on a novel and poems about chronic illness, it is difficult not to resent the slippery vocabulary that is given to us. I began writing when I could no longer dance ballet, because it seemed like something I could do no matter what happened to my body. Yet grasping at language to describe pain meant reverting to inadequate, cliched abstractions: I felt “attacked” by my body, which had already been spoken for. Looking at the blank page, I had “brain fog.”
Writing about pain can be an afflictive undertaking unto itself. In her poem “The Glass Essay,” which explores the end of a relationship as well as various dynamics between the Brontë sisters, Anne Carson writes:
It pains me to record this,
I am not a melodramatic person.
The act of admitting pain creates a new wound for the poem’s speaker — as it does for many writers attempting to articulate pain. Carson also makes a compelling case for metaphor in her poem “Essay on What I Think About Most”:
Metaphors teach the mind
to enjoy error
and to learn
from the juxtaposition of what is and what is not the case.
Metaphor is indeed a murky realm, yet fruitful transmissions of meaning are possible. When I talked about writing with another dancer whose career had been ended by illness and injury, he described the bodily sensation of no longer being able to dance such familiar movements as a loss of “muscular sanity,” an abstraction I still find incredibly useful.
Sylvia Plath, one of the best-known women-in-pain, described the act of writing from her life experience in a 1962 interview:
I think my poems immediately come out of the sensuous and emotional experiences I have, but I must say I cannot sympathise with these cries from the heart that are informed by nothing except a needle or a knife, or whatever it is. I believe that one should be able to control and manipulate experiences, even the most terrific, like madness, being tortured, this sort of experience, and one should be able to manipulate these experiences with an informed and an intelligent mind.
Plath’s warning against artless vulnerability brought Augustine to mind. Augustine was not a writer, but in creating her images and rising through the ranks of the Salpêtrière’s patients, she was surely crafting and manipulating her pain into something deliberate. Her expressions of suffering have since been lauded as an aesthetic accomplishment: André Breton called hysteria “the greatest poetic discovery of the late nineteenth century,” and printed photos of Augustine in La Révolution Surréaliste to commemorate “the fiftieth anniversary of hysteria.”
Still, finding the right words for pain is paramount. The “language” hysteria provided Augustine was ultimately insufficient, and playing the role of the medical pinup girl became more oppressive than her symptoms. She eventually refused to allow Charcot to hypnotize her, and gave a final expression of distress: the last entry in her medical file reads, “On September 9, Augustine escaped from the Salpêtrière, disguised as a man.”
¤
LARB Contributor
Emily Wells is the author of a memoir, A Matter of Appearance (Seven Stories Press, 2023). She teaches writing at UC Irvine.
LARB Staff Recommendations
The Intimate Life of Violence
Brad Evans speaks with Elaine Scarry, Walter M. Cabot Professor of Aesthetics and the General Theory of Value at Harvard University.
The Pain Woman: A Conversation with Barbara Gowdy
Gregg LaGambina interviews Canada’s hidden literary treasure, Barbara Gowdy.
Did you know LARB is a reader-supported nonprofit?
LARB publishes daily without a paywall as part of our mission to make rigorous, incisive, and engaging writing on every aspect of literature, culture, and the arts freely accessible to the public. Help us continue this work with your tax-deductible donation today!