To read more articles from LARB's "Around the World" section, click here.
All photographs by Allison Shelley. All rights reserved.
BIHAR, INDIA — Sugia Devi is moaning softly, reclined on a quilt-covered cot in a cramped room. The walls are indented with handprints from those who patted dirt layers into thick, insulating walls; it’s still chilly in the foggy morning hours. Dark blue scarves and blankets are wrapped around Sugia’s head and piled over her diminutive body, obscuring her swollen belly beneath the folds.
Next to Sugia, exhausted women huddle around a ceramic pot brimming with embers. Sunbeams stream through the decaying rice straw thatched roof, highlighting silky ribbons of smoke that prick their eyes.
A self identified “rural medical practitioner” — a semi-trained, independent health worker — hovers outside the feminine circle. He’s here to inject Sugia’s arms and thighs with oxytocin and Vitamin B to fortify her strength and speed her contractions. Labor is not progressing well.
A thick, loud woman named Malti Devi tromps into the room, breaking the silence with a litany of guttural greetings. Her face seems set in a constant grimace. Pushing aside the men she edges out the circle of women. She pours coconut oil over her fingers and inserts them into Sugia, checking the descent of the baby. Sugia squirms and tries to pull away.
But when Malti puts her ear to Sugia’s belly and murmurs “baccā ṭhīka hai” (“the baby is fine”), Sugia listens. Sugia repeats it back in her deep, clear, scratchy voice.
In this farming village in the impoverished north Indian state of Bihar, Malti is the birth czar. She handles a stethoscope, and assertively checks the position of the baby, massaging it into place. It is she who can say when it is time to go to the hospital. She is armed with success stories of reaching into a woman’s birth canal to push the baby back into position and stop it from coming out toward the anus. She has garnered respect and an ego to accompany it; almost everyone in the village has a story of her heroic deliveries.
In Bihar, 305 women die in childbirth for every 100,000 live births — among the highest rates in India — compared to only 28 deaths per 100,000 in the US. Nearly half of all pregnant women deliver at home, according to government statistics. When they do, they are often assisted by a traditional birth attendant, or TBA, like Malti. These frontline health workers straddle an uncomfortable role, essential in communities’ lives, but largely brushed to the side in the medical sphere.
They also pose a conundrum for global health strategists. The World Health Organization historically promoted training TBA’s, but they found there was little impact on maternal mortality rates. Still, “One has to respect TBA’s as part and parcel of life […] we have to work with them,” said Frances Day-Stirk, president of the International Confederation of Midwives. But mostly global health programs try to harness the social power TBA’s have and relegate them to educational tasks, steering them away from their central role handling deliveries.
“Now in India, TBA’s officially are not there,” said Dr. Manju Chhugani, dean of the Rufaida College of Nursing in the capital Delhi. She was sitting a world away from Malti and Sugia, perched on an orange couch in the Prague Congress Center, a brown-toned relic of the former communist regime. She was attending the International Confederation of Midwives Triennial Conference. Nearly 4,000 midwives were there, but they are official midwives, trained and certified, and there is a global shortage. According to the 2014 State of the World’s Midwifery report, around 70 percent of births in India happen with a skilled birth attendant. The births Malti attends would not be counted among those skilled deliveries, and as Chhugani said, Malti’s work is officially invisible.
In the hut, when Malti picks up her phone, she stares at it, squinting, then presses a button on the keypad. A jangling electronic voice announces the hour in Hindi. When she wants to make a call she hands a slip of paper and her phone to Nisa, one of the young teenagers hovering around the commotion. Nisa dials, and hands Malti back the mobile. Smoking a beedi — a hand rolled cigarette — and burping unapologetically, Malti hollers into the phone.
She is the most blaring, brash presence in the room, but she cannot read, even numbers. Her power and wisdom have nothing to do with education or literacy.
India is a hierarchical place, Bihar even more so. Untouchability — the ostracizing of social groups traditionally relegated to dirty tasks and excluded from many shared spaces — was outlawed in the 1950 constitution. But the effects linger, especially in distant reaches of the country. Malti comes from the Manjhi caste, a subset of the Dalit, or untouchables. In the hospital the social stratification is glaring.
In the hut, Sugia’s contractions start to slow; she is getting weaker and weaker. Malti decides it is time to go to the clinic. The family balks at the price — a delivery is 9,000 rupees ($151) in a state with an average per capita income of $324 that year — but no one considers taking her to the public hospital, which technically should be free. Public care is considered dangerous and deadly, private care expensive. It is only with Malti’s links to the private clinic that people trust her to go.
Malti works day shifts in the clinic between delivering babies at home and raising cattle. She has the doctors on call; for one complicated birth she called the doctor to come into the village. “People trust me because I have spent lot of time with doctors, they trust because I have gained knowledge from doctors so by any means I can get the delivery done. If delivery is not possible at home then I can also take them to doctor and get it done, that’s why people trust me,” she said.
A village elder, Chotani Manjhi, echoed her confidence, “We don’t trust [the government], we go to Prajapati hospital because we know Malti,” he said. “She does very good work,”
But while in the village her ties to the medical establishment strengthen Malti’s esteem, inside the clinic the power dynamic shifts sharply.
A pile of medical waste spills over the embankment on the side of the road outside. I asked where the waste goes; a curt junior doctor named Dr. Hare Ram Kumar said simply, “Malti.”
“Malti?” I ask.
“Malti moves it.”
Malti’s role at the clinic, exalted though it may be outside, is bloody. She cleans the room after the birth, wiping up the blood, scrubbing the floor. She transports the tainted waste. She works her bare hands, wearing a sari, while the doctors wear scrubs and gloves.
Yet even as she is relegated to the dirtiest tasks, the doctors rely on her to bridge the chasm between the elite western medicine and the birth traditions of the rural villagers.
Sugia’s labor stalled because the baby was breach. There was nothing Malti could do to deliver that baby naturally. Sugia ended up in surgery. But her anesthesia was not strong enough — she flailed in pain as they cut into her abdomen, and panicked. The doctors, consumed with the procedure, and annoyed at the disruption, called Malti to come in and quiet her. She was the only woman working in the room, called in to silence the emotions.
It’s because of complications like these that the government has programs to encourage women to deliver in the hospital. Around 15% of women globally have complicated deliveries; many of them happen suddenly, and need immediate care. Issues like hemorrhage and poor positioning can become deadly if a lengthy rickshaw ride stands between the laboring women and the hospital. And Malti, regardless of her self-trained expertise, cannot fix all the problems.
But the hospitals are seen as a place people go to die, doctors seen as oppressive and discriminatory; without a personal link, many families choose to avoid clinics at all cost. The government may be trying to edge risky home births to the side, but the essential connection between the community and medicine may well still live in the aggressive, awkward and illiterate figure of Malti and traditional birth attendants like her.
¤
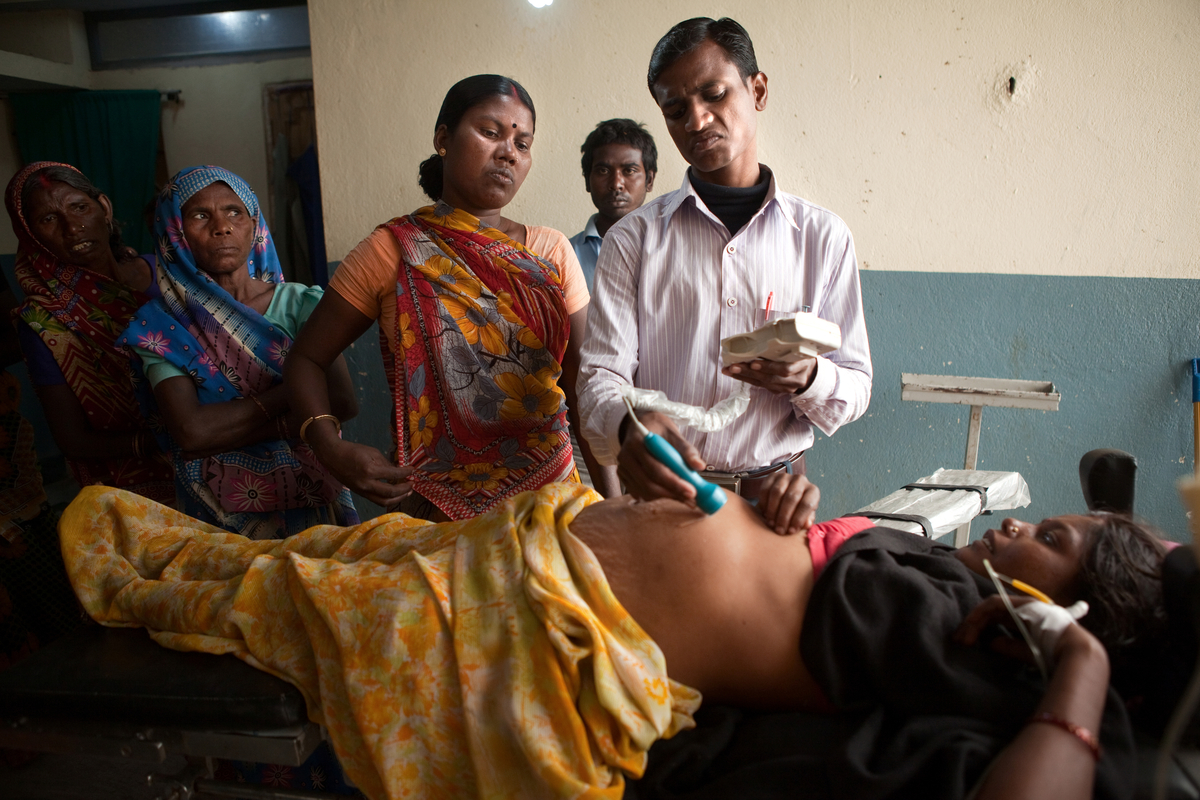
Dr. Sudhir Kumar, right, confers with traditional birth attendant Malti Devi, as they ascertain the condition of Muni Devi in labor with her first child at Prajapati Nursing Home in the town of Bodhgaya in the state of Bihar, India. The baby was sideways in the womb and was eventually born via Caesarian section.
¤
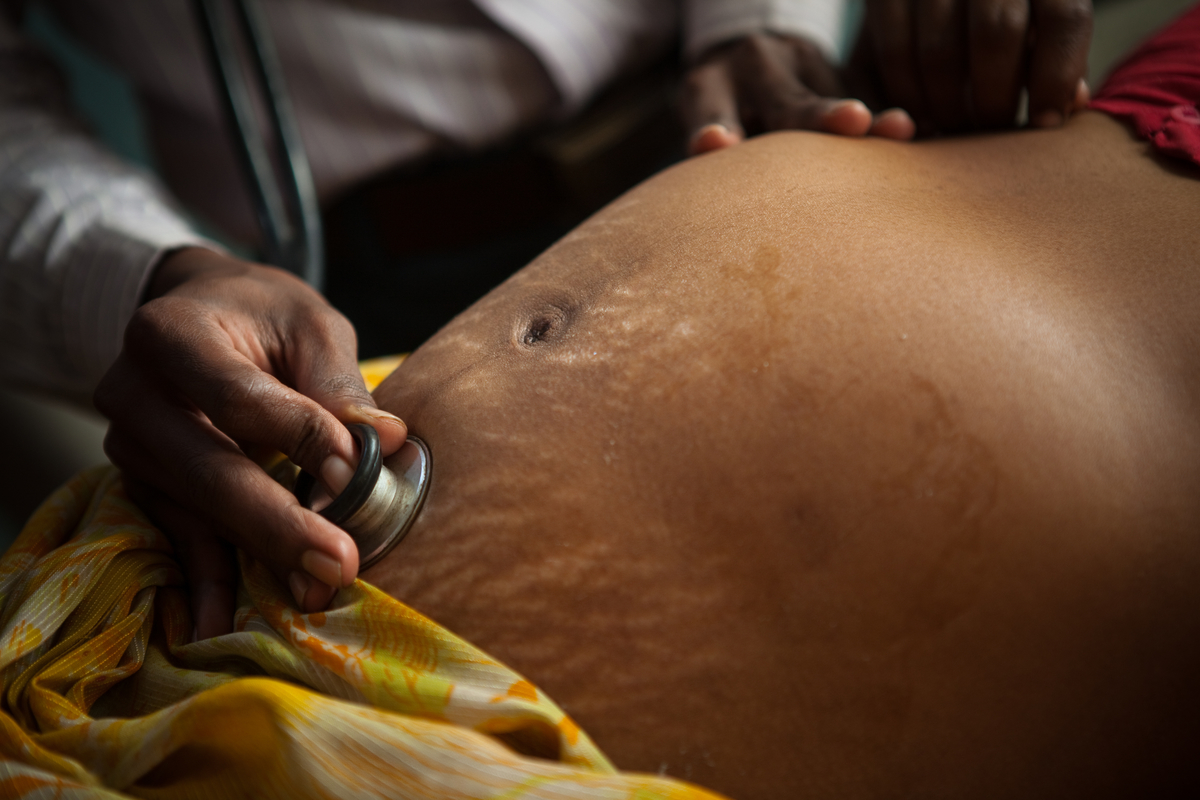
Dr. Sudhir Kumar ascertains the condition of teenager Muni Devi in labor with her first child.
¤
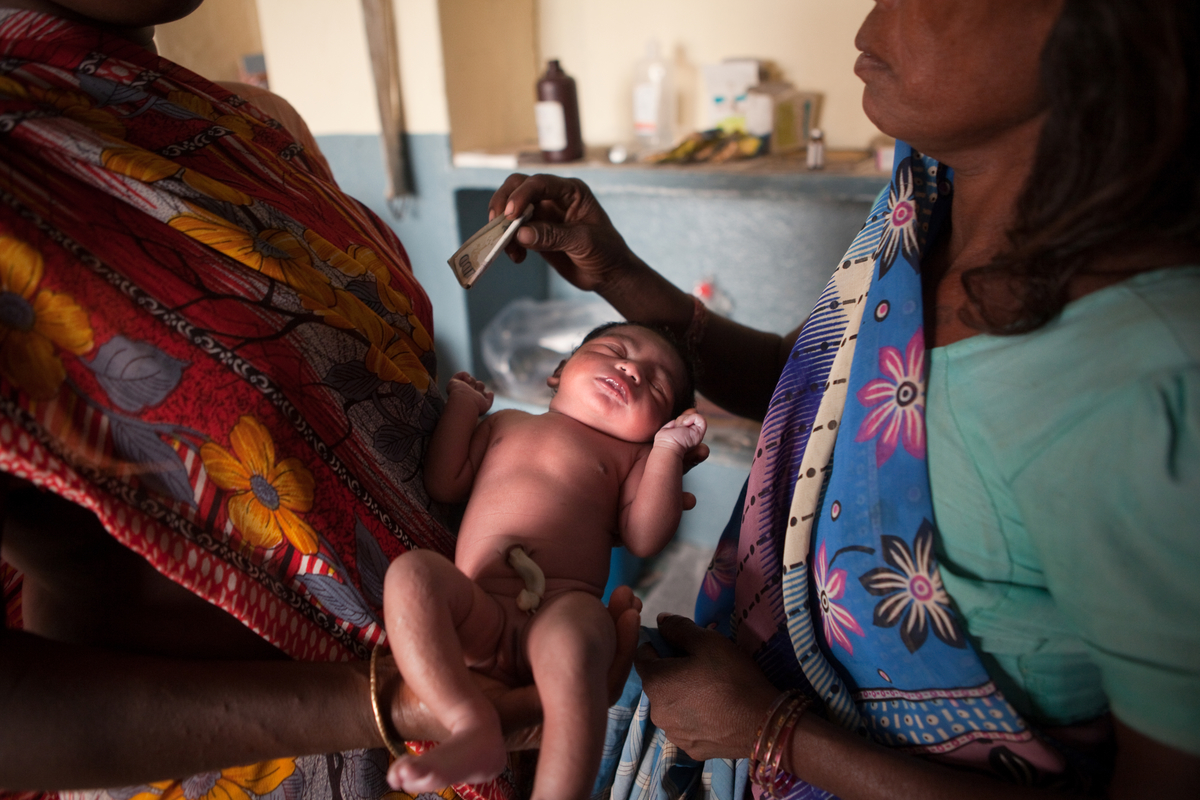
Muni Devi's newborn baby sits in the delivery room as traditional birth attendant Malti Devi, right, cleans up after the birth.
¤
Malti Devi, right, helps carry unconscious Muni Devi to a recovery bed.
¤
Malti Devi, left, is offered money for her help during the delivery by a family member of the new mother.
¤
Medical center staff lecture Malti Devi, a part-time employee, after Muni Devi, center, delivered her first child.
¤
Sugia Devi labors before dawn in the mud home where she lives with her husband's family in the village of Mounia in the state of Bihar, India. Sugia's labor lasted two full nights and involved three midwives and the village doctor. She eventually delivered a baby girl via Caesarian section in a local clinic — the second facility she was brought to, as the first did not have the necessary resources.
¤
Muna Devi, left, and Malti Devi, right, help Sugia Devi — Muna's sister — walk to a bicycle rickshaw as she labors in the village of Mounia in the state of Bihar.
¤
Malti Devi takes a break as Sugia Devi, below, labors in the mud home where she lives with her husband's family.
¤
This reporting was supported by the White House News Photographer’s Association.
LARB Contributor
Allyn Gaestel is a freelance journalist who covers human rights, inequality, gender, global health and the human repercussions of politics. She has worked in West Africa, the Caribbean, and Southeast Asia for outlets including The New York Times, The Washington Post, Al Jazeera, The Los Angeles Times, Reuters, and CNN and has received grants and fellowships from the Pulitzer Center, The International Reporting Project, The National Press Foundation, and others.
LARB Staff Recommendations
The Road Through Redemption Camp: Religion, Fertility and Abortion in Lagos
All photographs by Allison Shelley. All rights reserved. ON GROUND COOL WITH CONCRETE tiles, a woman carefully smoothed a turquoise and burnt...
Did you know LARB is a reader-supported nonprofit?
LARB publishes daily without a paywall as part of our mission to make rigorous, incisive, and engaging writing on every aspect of literature, culture, and the arts freely accessible to the public. Help us continue this work with your tax-deductible donation today!
:quality(75)/https%3A%2F%2Fdev.lareviewofbooks.org%2Fwp-content%2Fuploads%2F2014%2F06%2FINDIA_LARB_004.jpg)